
Managing ankle injuries
By: Holly Warner, PT, DPT
Are you suffering from weak ankles? Are you always rolling or spraining your ankles? Are you battling with foot/ankle tendon injuries? Try these exercises to improve your foot and ankle strength and stability.
Strength
Heel…
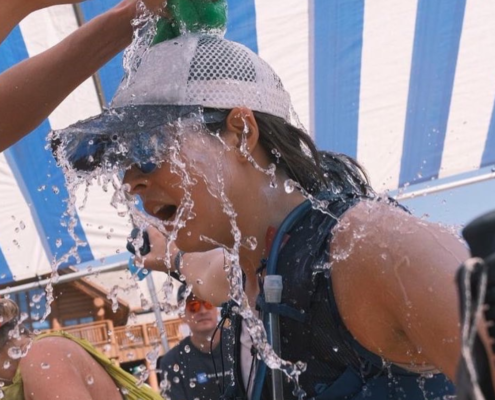
Performance Benefits of Heat Acclimation for Athletes
By: Adison Cook, SPT
Summers in Missoula continue to get warmer and for many that means setting the alarm earlier for their workouts. However, research shows that heat training can be very beneficial in preparation for…
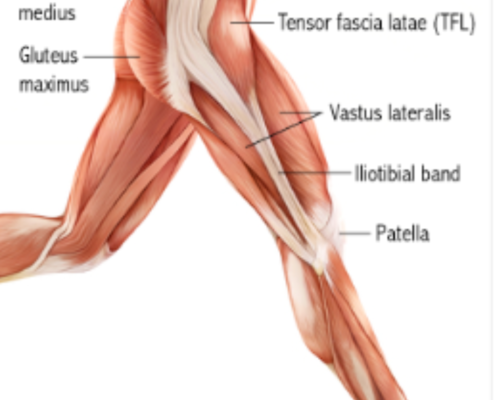
Understanding and Addressing IT Band Pain
By: Benjamin Blakely, PT, DPT, CSCS
Whether you enjoy biking, camping, hiking, or trail running, summer is the best time of year to live in Big Sky country and enjoy the outdoors. Here at Sapphire Physical Therapy, we work with a lot of patients…

Carbon fiber plated running shoes: are they right for you and your feet?
By: John Fiore, PT, Sapphire Physical Therapy
As runners, we are constantly on the lookout for the next great shoe, hoping to find the Holy
Grail of running shoes. I am guilty of owning an embarrassingly large number of running shoes. While…

Are calf raises the new anti-aging antidote?
By: Bailey Lodato, PT, DPT
Manual muscle testing has been a standard clinical measure used to assess muscle forces since the early 1900s by Lovett and Wright (1, 2). Originally developed in response to polio’s impact on muscular strength…

Understanding Knee Osteoarthritis
By: Erin Williams, PT, DPT
Knee Osteoarthritis: To run or not to run?
We gravitate toward running because of many wonderful benefits. To name a few, running maintains heart, lung, muscle, tendon, and bone density health - and that’s just…


